
 Dr. Carolyn Steele Gray
Dr. Carolyn Steele Gray
By Marcia Kaye
Putting simple but innovative technologies in the hands of patients with complex care needs may lead to better health outcomes, according to new research from an innovation scientist.
It can be as simple as a mobile app, says Dr. Carolyn Steele Gray, a Scientist at Bridgepoint Collaboratory for Research and Innovation, part of the Lunenfeld-Tanenbaum Research Institute at Sinai Health System. Dr. Steele Gray studies ways to use digital technologies to improve care for individuals with several chronic illnesses — an area of focus at Sinai Health. She has been developing and testing a phone app and web portal that helps providers and patients work together to set care plans based on patients’ own personal health goals. Primary care doctors, allied health professionals, patients and families can collaboratively monitor the process and tailor care delivery to patient priorities — a very different approach from the traditional model of care.
“Rather than a provider saying to a patient with five or six chronic conditions, ‘Let’s tightly manage all of those things,’ the patient comes in and says, ‘I want to get out to my social events more often,’ or ‘I want to walk my dog,’ and then the care plan gets focused on that,” explains Dr. Steele Gray. The technology helps patients track progress; for instance, for a patient whose goal is to golf three times a week, the app will ask, “How was your pain when you went golfing today?” and “How many steps did you take?” Patients check off completed tasks and receive virtual badges. The tool, called ePRO — electronic Patient Reported Outcomes — gives doctors a wealth of data.
In an exploratory four-month trial with 16 patients in two sites, the researchers found that as patients focused on their own personal goals, their general health improved too, including lower blood pressure, healthier weight and better sleep. “A lot of health indicators were improving because people were engaging in activities that were meaningful to them, which can improve their outcomes over the longer term,” she says.
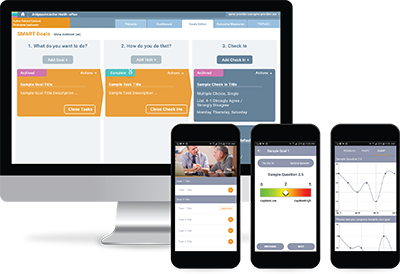 ePro, an app developed by Dr. Steele Gray and her team, allows patients to record their health goals and track their progress
ePro, an app developed by Dr. Steele Gray and her team, allows patients to record their health goals and track their progress
Dr. Steele Gray says that while some tech-savvy patients initially thought ePRO was too simplistic, they ultimately found it helpful and fun. Some providers were initially reluctant to add a new piece of technology to their busy schedules, but their patients’ good results won them over. It’s hoped that ePRO will save money by reducing patient visits to doctors and hospitals. The tool is now in trials with nearly 50 patients and their doctors across Ontario.
Looking more broadly, Dr. Steele Gray is interested in using digital technologies to better connect patients and family doctors with specialists, home care providers and hospitals. She says that better integration of information can reduce duplicate testing and medication errors, and improve patient care. For instance, Ontario has a dozen different types of electronic medical records, with no centralized system. In a recent study, she found that even when providers were using such technology, they were simply supporting business as usual. “Most were using it exactly like a paper filing system, but there are more innovative ways you can use that kind of information, like doing disease management planning.”
She says that many technologies are developed by “very smart engineers who are often divorced from the health-care system,” which makes them challenging for health professionals to use. She says, “When we’re developing our mobile technologies, we don’t come in with a technology and say, ‘What do you think?’ We sit down with the people who would use it and say, ‘What do you need?’ And then we build it with them step by step.”
She and her team are currently building a collaboration in Nova Scotia that will explore how to integrate mobile technologies on a provincially based patient health record platform. She’s also involved in the Europe-based International Federation of Integrated Care (IFIC), which holds conferences and trains people in improving integration across health-care systems. Building on her partnerships with Kaiser Permanente in Colorado and universities in Edinburgh and Glasgow, she’s starting an IFIC Special-Interest Group on digital health-enabled integration, which will build a community of practice around the development, implementation and evaluation of digital solutions that support integrated care to improve knowledge and technology sharing across countries.
Photo credit John Packman