
Written By: Marcia Kaye
Photos By: John Packman
When you think “orthopaedic surgery,” what springs to mind? Probably a hip or knee replacement of an aging joint. But that’s only one part of a very large picture. In fact, Sinai Health System treats a wide variety of orthopaedic needs and patients, including young people, athletes and others in their prime who may have suffered sports injuries, illness or accidents.
The Granovsky Gluskin Division of Orthopaedics at Mount Sinai Hospital, part of Sinai Health System, performs more than 700 surgeries a year, many of them on patients under the age of 50, and some under 20. Led by Dr. David Backstein, who is consistently named by Canadian and U.S. colleagues as one of the top knee surgeons in North America, it has become a power hub of orthopaedic surgery, with a team of world-renowned experts with particular skill in complex and even unique procedures. Combined with the expertise within the ortho rehab program at Bridgepoint Active Healthcare, part of Sinai Health System, the multidisciplinary orthopaedic care teams help facilitate seamless care, helping patients of all ages return to active and engaged lives.
Meet three recent orthopaedic patients — a teenage ski racer, a young cancer survivor and a midlife patient who had an unlucky fall — and find out how we helped them all get back on track.
It was the final run of the day, and 15-year-old Maddy Sullivan was in fine form last November as she executed precision turns at electrifying speeds down the giant slalom course on Austria’s magnificent Hintertux glacier. But suddenly, on a sharp left turn, Maddy’s gloved hand got hooked between the double poles of the gate. That swung her back, causing her right ski to twist outward as her body still pointed inward. As she fell, she sensed a pop in her knee. “I can still remember feeling it tear,” she says.
 Maddy, an elite ski racer who had reached the highest possible level for her age — she won the Nancy Greene Award at the international Whistler Cup at 13 — had suffered her first-ever injury: an ACL tear. A tear of the anterior cruciate ligament typically happens when the upper leg and lower leg twist in opposite directions. It’s the most common injury in teenage athletes, who often put superhuman stresses on young knees.
Maddy, an elite ski racer who had reached the highest possible level for her age — she won the Nancy Greene Award at the international Whistler Cup at 13 — had suffered her first-ever injury: an ACL tear. A tear of the anterior cruciate ligament typically happens when the upper leg and lower leg twist in opposite directions. It’s the most common injury in teenage athletes, who often put superhuman stresses on young knees.
Flying back to Toronto two days later with her mom, Maddy was determined to do whatever it took to get back to the sport she loves. A consult with Sinai Health System’s orthopaedic surgeon Dr. John Theodoropoulos — known to his patients and colleagues as “Dr. Theo” — revealed she would need not just a repair but a reconstruction: a new ACL. To optimize her surgical outcome, Maddy underwent close to a month of pre-op physiotherapy to eliminate swelling and regain her full range of motion.
Typical ACL reconstruction options include using a patient’s own tendon (taken from the hamstring or kneecap) or a cadaver tendon, but in this case Dr. Theo and Maddy made the decision to use her own kneecap tendon, even though it would mean a more painful recovery. “For my elite athletes I like to use a patellar tendon because it’s a stronger graft that can withstand the increased stress these young athletes put on the knee,” says Dr. Theo, who is also the orthopaedic surgeon for the Toronto Maple Leafs and Toronto Blue Jays. He removed the middle third of Maddy’s kneecap tendon, with a bone plug on each end from her kneecap and tibia, and fashioned a brand-new ACL, reattaching the graft with screws on either end.
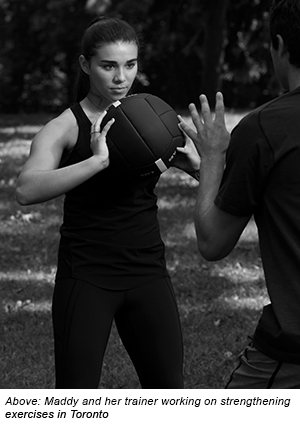 Dr. Theo kept Maddy informed every step of the way, just as he does with his pro athletes and other patients. He discussed surgery details with her, kept her updated with the latest research on recovery timelines and talked about the anxiety athletes can feel when they return to play.
Dr. Theo kept Maddy informed every step of the way, just as he does with his pro athletes and other patients. He discussed surgery details with her, kept her updated with the latest research on recovery timelines and talked about the anxiety athletes can feel when they return to play.
“Every time I met with Dr. Theo, we had conversations that weren’t just about my knee,” Maddy says, “but about how it was relative to my life — skiing is a big part of my life — and how it impacts the things that are important to me.” She adds, “Surgery is a scary thing to think about, but I wasn’t feeling any of those fears because everyone was very informative and helpful and considerate, and they just wanted to put my best interests ahead of everything else.”
Dr. Theo, who works with a team of athletic therapists, physiotherapists, strength coaches and nutritionists, says his biggest challenge with Maddy, as with other elite athletes, was to hold her back from doing too much too soon. But after a nine-month physio program, with her new ACL at least as strong as her old one was, Maddy was cleared to head back to the ski hills. A member of the Ontario Ski Team, she’s currently training in Switzerland to prepare for the racing season, which begins in December.
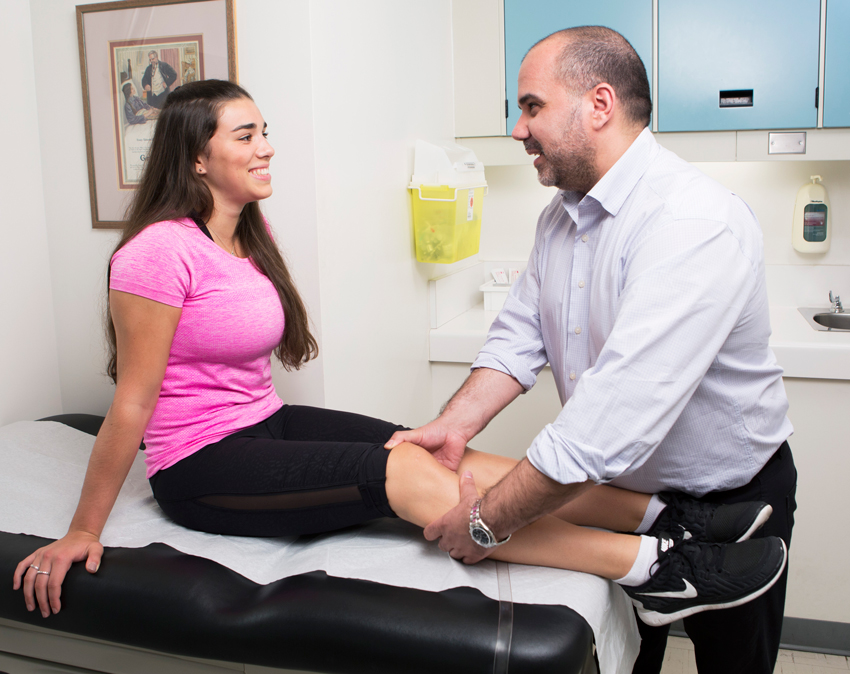 Above: Maddy with Dr. John Theodoropoulos, Orthopaedic Surgeron
Above: Maddy with Dr. John Theodoropoulos, Orthopaedic Surgeron
“She’s going to be a supertalent like Lindsey Vonn,” predicts Dr. Theo, referring to the U.S. ski sensation who came back after similar ACL surgery to win a World Cup.
On reflection, Maddy says it wasn’t too big a deal to miss last year’s racing season. “I’m still really young, and there’ll be tons of races,” says the eleventh-grader, now 16 and with an eye on future Olympic Games. “I’m nothing compared to what I’ll do in the future.”
As a teenage survivor of cancer, Rohit Mathews was just getting his life nicely back on track. The 18-year-old was studying paramedicine at University of Toronto Scarborough and working as a lifeguard. Two years earlier he’d been treated for Hodgkin’s Lymphoma, a cancer of the lymphatic system, and was cured. Life was good — until Rohit noticed some pain in his right hip.
At first he attributed it to muscle strain from his daily bicycle commute. But when the soreness became unbearable — “I was in so much pain I couldn’t put my socks on” — his mom, a nurse, insisted Rohit get an X-ray. The surprising diagnosis: avascular necrosis to the femoral head. In other words, the bone tissue at the top of Rohit’s thigh bone — the ball that fits into the hip socket — had begun to die.
The cause became clear. His course of cancer treatment, which involved four months of chemotherapy and one month of radiation, had also included high doses of prednisone, a corticosteroid that can boost the efficacy and reduce the negative side effects of chemotherapy. Unfortunately, long-term high-dose prednisone can sometimes cause reduced blood flow to joints. Rohit was free of cancer but had essentially lost a hip.
 Above: Rohit with Dr. Paul Kuzyk
Above: Rohit with Dr. Paul Kuzyk
Conventional hip replacement involves a titanium-and-polyethylene prosthetic, but in young patients there are caveats. Despite better materials, coatings and contours, the implants last only about 20 years, with each successive implant becoming a trickier surgery.
Doctors at Mount Sinai offered Rohit a better option: a fresh osteochondral allograft. This would involve harvesting bone and cartilage from a recently deceased donor and transplanting them into his hip. Mount Sinai is one of the only centres in the world doing such a procedure on hips. It has now done 23 procedures.
“In Rohit’s case we used a large graft from a donated hip and put it into his hip in the area where the ball had collapsed,” says Dr. Paul Kuzyk, the orthopaedic surgeon who performed the delicate procedure. It worked. No one can predict with certainty how long it will last, because there’s no long-term data yet, but Dr. Kuzyk says, “It has the potential to last forever. But it’s a win if it even lasts 10 years, because it gives him 10 years of pain-free activity before he has to have a hip replacement.”
“I’m physically active, I can walk an unlimited amount of kilometres, I ride a bike,” says Rohit. “I had a full-time summer job in golf operations at a country club that required me to carry stuff, and my femur is holding strong.”
- Rohit Mathews, Patient
And by then, there may be even better options. Clinician-scientist Dr. Rita Kandel, Chief of Pathology and Laboratory Medicine at Sinai Heatlh System, and her research team are working on using stem cells through 3D printing to build replacement joints not of metal and plastic but from a patient’s own cells and tissues. If successful, the promising technology has the potential to revolutionize orthopaedic medicine.
In the weeks following the surgery, Rohit did the prescribed exercises — with a lot of motivation from his mom — and it paid off. After three months he was walking unassisted. Today he’s pretty well back to normal. “I’m physically active, I can walk an unlimited amount of kilometres, I ride a bike,” he says. “I had a full-time summer job in golf operations at a country club that required me to carry stuff, and my femur is holding strong.”
Although Rohit, now 20, has gone through two serious medical conditions, he has nothing but gratitude for his current state of good health and the medical team that helped him get there. “I’m really grateful for the work the doctors did. The staff were very good, the physiotherapist was super helpful and Dr. Kuzyk himself was a really good orthopaedic surgeon. He was really kind, too. He’s a good guy.”
There was one disappointment. Rohit had to give up his long-held ambition of becoming a paramedic, since the physical demands would overly stress his hip. “That was a bummer,” he admits. Instead, he switched majors and is now in his second year of forensic science at University of Toronto Mississauga. “I’m definitely enjoying it. I have no regrets.”
People sometimes fall into a new job. For Charles Shorrock, that happened quite literally. It was an actual physical fall that led the former sales and customer service manager into an entirely new career as a patient advisor at Sinai Health System.
On a Friday evening last October, Charles, 45, was walking down three flights of stairs from a friend’s Toronto apartment. He’d arrived on the bottom stair when for no apparent reason — the stair was sound, the lighting was good and he wasn’t on his phone or otherwise distracted — he stumbled and fell onto his hands and knees on the lobby’s hardwood floor. He instantly felt a fiery sensation spreading up from his knees. “The pain was so sudden and intense I couldn’t breathe,” he recalls. His legs wouldn’t move. His phone had bounced out and skittered across the lobby, so he couldn’t even call for help.
 Above: Charles with Dennis Ng, physiotherapist at Bridgepoint Active Healthcare
Above: Charles with Dennis Ng, physiotherapist at Bridgepoint Active Healthcare
Fortunately a passerby spotted Charles through the building’s glass front doors and called 911. When the paramedics asked Charles if he had a preference among three equidistant hospitals, he immediately said, “Mount Sinai!” He’d visited Sinai’s Schwartz/Reisman Emergency Centre a few years before and says, “I was blown away by the care and consideration I got in the ER, and I was so impressed at how well the staff flowed and how they engaged with patients.” He was also a user of Sinai’s family medicine program.
Charles was triaged right away. Medical imaging showed that his injury was a devastating one: complete bilateral quadriceps tendon rupture. His one-stair tumble had torn the tendons in both knees, effectively severing the four quad muscles in his upper legs from his lower legs.
A common repair involves connecting the muscles to fibres on a metal plate drilled into the knee. But because of Charles’s young age, the surgeons chose to suture together the trimmed edges of the torn tendons. It would extend his recovery time but minimize the long-term impact on his knees. To ensure healing, his legs would need to be in splints, locked straight, for most of the next 14 weeks.
“It’s miraculous. If I saw him on the street I would never have known he’d had those injuries.”
- Dennis Ng, physiotherapist at Bridgepoint Active Healthcare
Three days after his surgery, and just a week after his fall, Charles was relocated to Bridgepoint for rehabilitation. Since he wasn’t allowed to bend his knees, his exercises included a stiff-legged “Frankenstein” walk with a walker, standing on tiptoes and small leg swings — or as Charles calls them, “ballet barre exercises” — using the waist-high railings in Bridgepoint’s hallways, which are active therapy areas. His physiotherapist, Dennis Ng, says these small movements made a big difference in helping Charles achieve his therapy milestones quickly: “It’s all about trying to maintain the strength that you have.”
Once the splints were off, Charles could begin bent-knee exercises. Dennis and Charles’s occupational therapist also went with Charles to his house, which has narrow doors and steep staircases, to assess when he could safely return home.
Charles had to give up his old job of demonstrating and selling heavy commercial restaurant equipment. But during his 15-week hospital stay, he became a very engaged patient. Having spent seven years improving and restructuring customer service processes for a global information company, Charles became interested in the quality improvement process for patients, families and caregivers. Last March, soon after he was discharged, he was hired as Sinai Health System’s first-ever patient advisor on staff. His latest initiatives involve orientation sessions for patients and families, engaging patients for trial projects and training staff in patient and family engagement.
Today Charles goes for walks every evening, cycles two or three times a week and even does a little yoga at home. “I’m more flexible than I ever was because I’m consciously doing stretching,” he says.
Dennis, who often sees Charles at work now, says, “It’s miraculous. If I saw him on the street I would never have known he’d had those injuries.”